WHY THIS MATTERS IN BRIEF
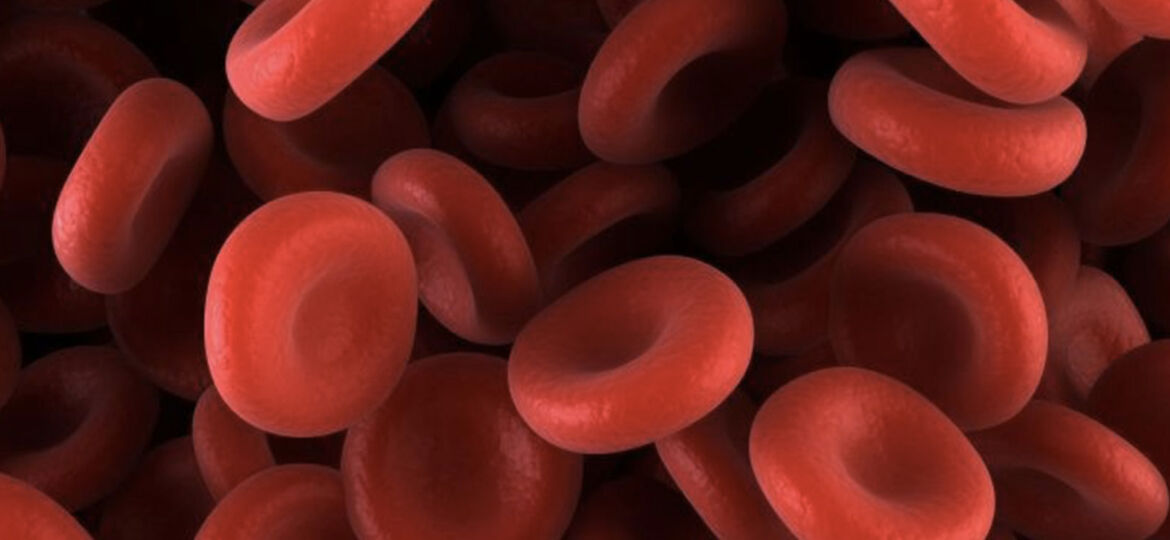
Hundreds of millions of people each year need some form of blood transfusion and supplies are always stressed, this latest breakthrough could let doctors produce any type of blood on demand and save countless lives.
Researchers at the University of Bristol (UB) have made a major breakthrough in the creation of artificial blood cells that could one day lead to the production of mass produced blood – an area that the US Army recently announced they’re also now also going to be researching.
The team from the university worked alongside researchers from NHS Blood and Transplant to create a radical new process that has allowed them to mass produce artificial blood on a scale never seen before, and the breakthrough came after the team were able to make use of early stage stem cells, also known as “Immortal cells” to grow billions of red blood cells.
At present, the only way to produce artificial blood is to grow donated stem cells directly into blood cells. This is slow, inefficient and requires repeat donations in order to be of any feasible use, so as a consequence it’s only used in exceptional circumstances.
What the researchers did instead was to trap stem cells in an early stage of their development where they can multiply an unlimited number of times.
A typical stem cell can produce just 50,000 red blood cells before dying out, but these immortal cells can multiply endlessly allowing for much, much larger quantities to be produced, and artificial blood produced in this way has a number significant benefits over donated blood.
“Globally, there is a need for an alternative red cell product. Cultured red blood cells have advantages over donor blood, such as reduced risk of infectious disease transmission,” explained Dr Jan Frayne, from the university’s School of Biochemistry.
While this is a major breakthrough, unfortunately we’re not going to be seeing mass produced artificial blood appearing in hospitals anytime soon, and it’s certainly not because they aren’t needed because once the technology is ready the demand will almost likely immediately outstrip supply.
“The first therapeutic use of a cultured red cell product is likely to be for patients with rare blood groups because suitable conventional red blood cell donations can be difficult to source,” said Professor Dave Anstee, Director at the NIHR Blood and Transplant Research Unit.
“The patients who stand to potentially benefit most are those with complex and life limiting conditions like Sickle Cell Disease,” which had its own breakthrough recently when researchers announced a cure, said Anstee, “and Thalassemia, which can require multiple transfusions of well matched blood. The intention is not to replace blood donation but provide specialist treatment for specific patient groups.”
















Thank you Mathew for the informative article! New trends in medicine, especially ones that have immediate application for current patients, need a larger voice. We look forward to sharing more of your articles. Here in Silicon Valley, we have recently launched a new non-profit initiative called CrowdHealing, which will create central global conversations for hundreds of diseases and medical topics through expert panels and monthly webinars, to give the new treatment possibilities a louder voice to the patient community, and expedite new breakthroughs to the clinical setting through patient demand. I think this would be something that you would enjoy learning more about. Please visit our website http://www.WeHeal.org or contact me directly.
Thanks Eric, glad you liked it – there’s so much going on in healthcare at the moment it’s a wonderful space to watch. I’ll have a look at your site, anything that helps improve people’s lives, and quality of life is to be applauded, I’ll ping you.