WHY THIS MATTERS IN BRIEF
Medical supply chains are incredibly complex and highly regulated but now we’re on the cusp of 3D printing human organs and prosthetics on demand, and medicines are following suit.
Medicine gets a lot of attention, but normally it’s to do with drug development rather than drug manufacturing, and the last time drug manufacturing got a boost was when a Scottish researcher managed to demonstrate how his “Chemputer,” a very promising molecular assembler technology that’s now being used to grow basic drones in the defence industry, could assemble simple drugs such as painkillers and Aspirin.
Now though, by adapting a technology used to manufacturer electronic components, researchers at the University of Michigan have developed a new way to manufacture medication, and the new technique could eventually let hospitals, pharmacies and doctor’s offices eliminate their pharmaceutical supply chains and print, and mix, drugs on demand into one single easy to administer dose.
3D Printing and healthcare have tangoed before though, for example, the FDA has already approved a technique for 3D printable drugs that are more easily absorbed by the body thanks to their porous nature, and over the last few years we’ve also seen plenty of advances in 3D printed human organs, implants and a whole manner of other things besides.
This latest technique was adapted from a process called organic vapour-jet printing, a method of manufacturing electronics that lets users deposit fine crystals of a material onto a substrate. In order to print their medication, the team heated a powdered form of an active pharmaceutical ingredient until it evaporated and then combined with a heated inert gas that was then funnelled through a nozzle and deposited onto a chilled surface, where it cooled to form a thin crystalline film.
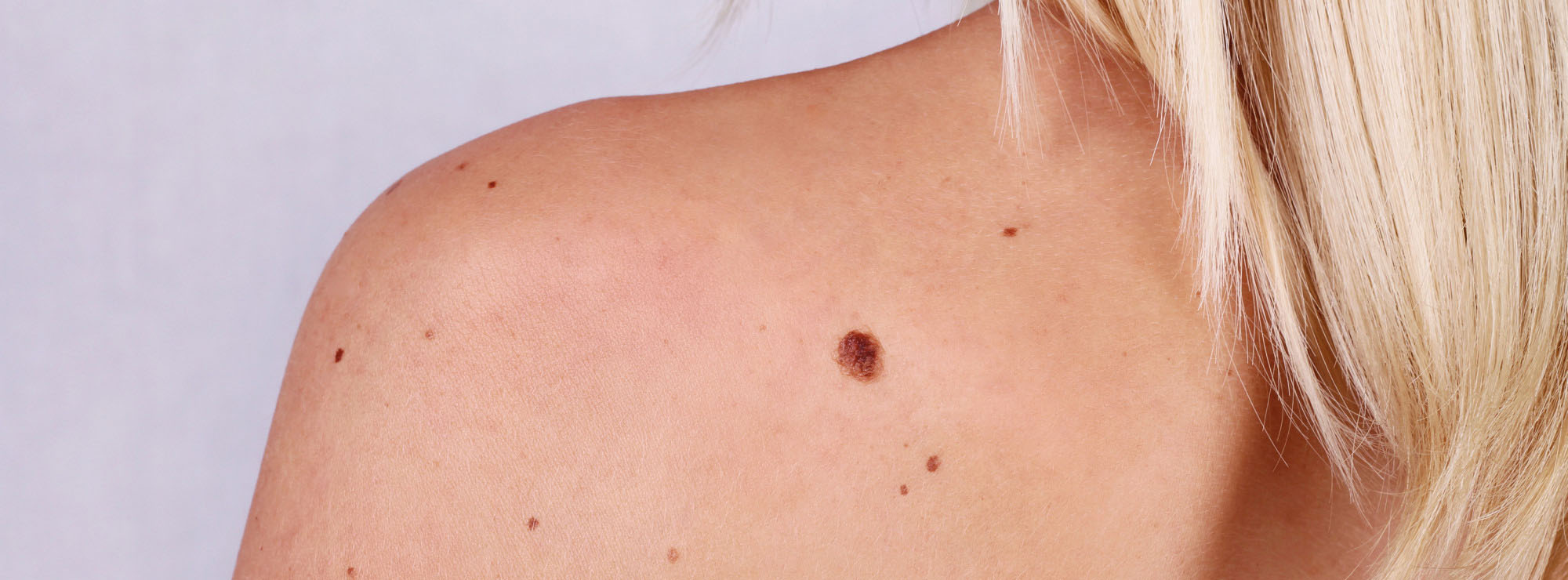
Furthermore, in their tests, the researchers showed that medication printed in this way was just as effective at killing lab grown cancer cells as other medication, but that said it also turns out that there are some other added advantages to using this technique.
According to the researchers, it also allows the drug to dissolve more easily without having to add other solvents or chemicals to the mix, which not only helps the patient absorb the medicine faster but could also help drugs pass the rigorous screening processes that often stand between them and mainstream adoption.
“Pharma companies have libraries of millions of compounds to evaluate, and one of the first tests is solubility,” says Max Shtein, lead researcher on the study, “about half of new compounds fail this test and are ruled out. Organic vapour jet printing could make some of them more soluble, putting them back into the pipeline.”
Improving solubility also means that drugs behave in the lab more like they would in the body, making drug research more accurate and speeding up certification, and then, in the long run, the technique could also allow medications to be mixed and matched before being printed on site in pharmacies and hospitals onto a delivery device like a dissolvable strip or micro-needle patch.
“A doctor or pharmacist can choose any number of medications, which the machine would combine into a single dose,” says Shtein, “the machine could be sitting in the back of the pharmacy or even in a clinic.”
The research was published in the journal Nature Communications.