WHY THIS MATTERS IN BRIEF
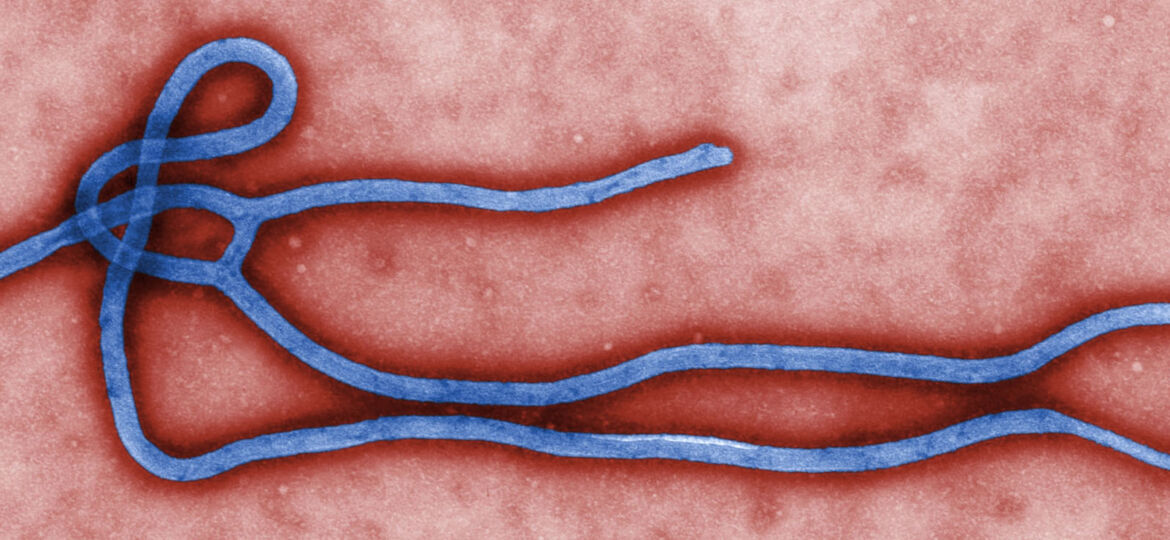
- Ebola has one of the highest mortality rates of any known virus and in the summer of 2016 it killed nearly 12,000 people – now we have a vaccine that’s 100% effective
Earlier this year the President of Sierra Leone called my brother-in-law, Robert Verkerk, the founder for the Alliance for Natural Health International, in to ask him to help the country deal with its worst Ebola outbreak in living memory, and the stories from the front line made many of the news reports, even the most harrowing ones, look mild by comparison. Now, after four decades of research, scientists have finally developed an effective vaccine in the fight against one of the world’s most virulent, indiscriminate, deadly diseases.
Research, published in The Lancet, describes a vaccine that provides complete protection against the disease. The trial was led by the World Health Organisation (WHO).
“Vaccine efficacy was 100%,” said the scientists behind the rVSV-ZEBOV vaccine.
While the vaccine isn’t yet approved by any regulatory authority for widespread use, in the trial of the vaccine in Guinea, West Africa, none of the 5,837 residents who received it contracted Ebola 10 or more days later. People who fell ill within the first nine days were discounted as it was assumed – given the incubation period of the disease – they had been infected before the vaccination was given.
Ebola is a devastating disease that during the 2013 to 2016 Ebola outbreaks in Africa took the lives of 11,300 people.
“While these compelling results come too late for those who lost their lives during West Africa’s Ebola epidemic, they show that when the next Ebola outbreak hits, we will not be defenceless,” said Dr Marie-Paule Kieny, WHO’s assistant Director General for Health Systems and Innovation.
In the event of another Ebola outbreak over 300,000 samples of the vaccine have been stockpiled and the it’s now being fast tracked through regulation.
The WHO said the trial of the vaccine used a method – dubbed “ring vaccination” – that was first tested with small pox. A ring of people who had been in contact with someone diagnosed with Ebola was identified, with adults over 18 being given the vaccine. After initial results showed it was proving successful the vaccine was given to all within the 117 rings, which were made up of an average of 80 people.
“In addition to showing high efficacy among those vaccinated, the trial also shows that unvaccinated people in the rings were indirectly protected from Ebola virus through the ring vaccination approach,” WHO said.
Those who received the vaccine were observed for 30 minutes and then had repeated home visits for 12 weeks. There were no long term effects but half the people vaccinated had headaches and fatigue shortly after being vaccinated. Previous tests of the vaccine in monkeys had protected them even when they were given a dose of Ebola a week later.
Although Ebola was first discovered in 1976, a vaccine has not been developed to date due to the limited impact before 2014. In the years preceding this, around 1,300 people died of the virus.
August 2014 saw the virus described as a “serious threat” and the WHO made it an “extraordinary” health event. This tag was removed by the WHO in March 2016, with the organisation says it “no longer constitutes” a public health emergency of international concern.
Peter Piot, who discovered the Ebola virus during the 70s said earlier this year the 2014 epidemic took people by surprise – describing it as the perfect storm and he criticised the WHO for being slow to act and said the world needs to be ready for the next big epidemic. And in July 2015, the WHO was criticised for its response to the spread of Ebola.
Oxfam chief executive Dame Barbara Stocking, in an independent report, said the WHO lacks the “capacity and culture” to face global health emergencies.
“You are always trying to prevent a situation coming through or grab it when it starts and really get it under control very fast and those are some of the internal changes that have to be made at WHO,” she said at the time.