WHY THIS MATTERS IN BRIEF
One step for a robot, one giant leap for robot kind.
In a recent study Oxford University and others estimated that between 35% and 45% of all of todays’ jobs would be automated by AI, robots and, or, software robots (bots) within the next twenty years. When asked what jobs us mere humans might occupy in the future the answers invariably involved jobs that value traits not found in our robotic counterparts such as creativity, empathy and dexterity but we’re already seeing signs that even those jobs are being automated. We’re already seeing significant advances in the area of creative, innovative machines and now robots are proving that they’re a match for us in the operating theatre – an environment where, arguably dexterity is one of the most highly valued traits.
Meet STAR
In a world first and a robotic surgery breakthrough, a robot has successfully stitched up a pig’s small intestines using its own vision, tools, and intelligence to carry out the procedure. What’s more startling though is that the Smart Tissue Autonomous Robot, or STAR for short, easily outperformed its human equivalents who were given the same task. In fact if it had been a soccer match then you could easily have argued that the score would have been 10-0.
STAR’s inventors don’t claim that robots can replace humans in the operating room anytime soon, although no doubt that’s on their minds. Instead they see the accomplishment as a proof of concept – both for the specific technologies used and for the general concept of “supervised autonomy” in the OR.
Pediatric surgeon Peter Kim, one of the researchers, didn’t sound threatened when he spoke to reporters in a press call yesterday. “Even though we surgeons take pride in our craft at doing procedures, to have a machine that works with us to improve outcomes and safety would be a tremendous benefit,” he said.
For this study, published today in the journal Science Translational Medicine, researchers programmed their robot to carry out a procedure called intestinalanastomosis, in which a piece of intestine that’s been cut through is stitched back together. It’s like repairing a garden hose, said Ryan Decker, the senior engineer on the team, in that the sutures must be tight and regularly spaced to prevent leaks. STAR performed this task both on ex vivo tissue in the lab and on in vivo tissue in an anaesthetised pig, and experienced human surgeons were given the same tasks. When the resulting sutures were compared, STAR’s stitches were more consistent and more resistant to leaks.
The robot did have a little help though. In about 40 percent of its trials, the researchers intervened to offer assistance of some sort such as holding the thread (it’s good to know that some surgeons might still be needed even if it is only to hold their robot masters’ needle and thread!) but in the other 60 percent of trials, STAR did the job completely on its own.
The researchers don’t think these assists invalidate their claim of autonomy; instead they see the setup as representative of shared control setups that would be appropriate for real ORs. Human surgeons could supervise procedures or even trade off tasks with the robot, letting the machine do more routine or tedious parts of an operation. “You can imagine that if something critical is happening, that would be a point where the surgeon is going to be closely monitoring the robot,” Decker said. “I’m sure they wouldn’t feel comfortable just letting it run and going to take a coffee break.”
Today, some surgical procedures already incorporate smart machines. Robots routinely carry out the crucial steps in some procedures including orthopedic knee replacements, Lasik eye surgery, and hair transplants. What these types of surgery have in common, though, is the fixed nature of their targets, as leg bones, eyes, and heads can be held in place during the procedure. Soft tissue surgeries are much messier and more difficult to automate, because all the slippery pink parts of the body shift around and are hard to track.
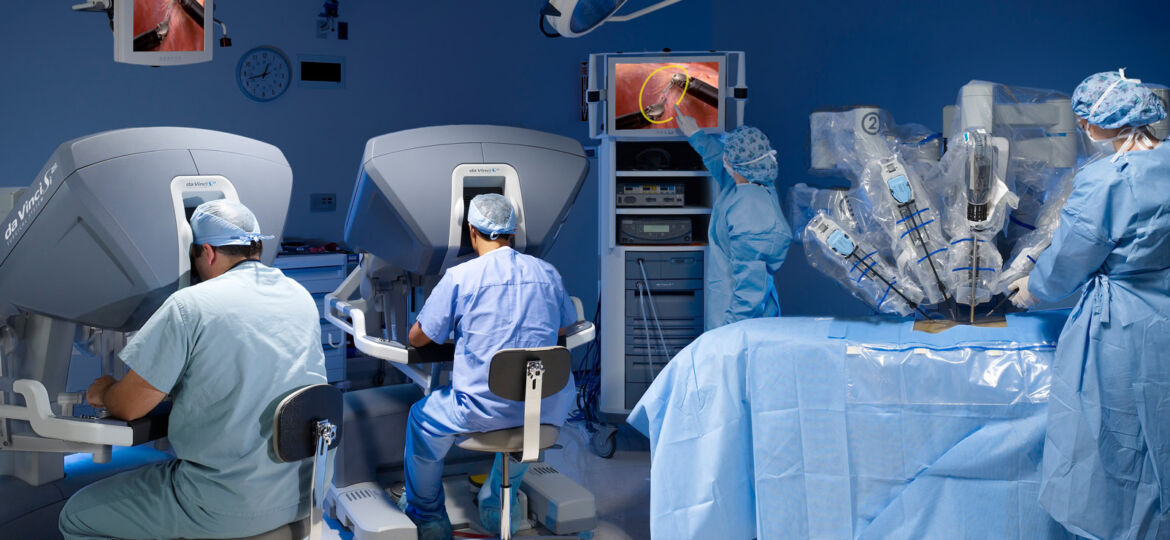
The current state of the art robot for soft tissue surgery is the da Vinci system from Intuitive Surgical, but it’s not automated at all. The da Vinci is a teleoperated system, in which the surgeon sits at a console and manipulates controls in dexterous manoeuvres that are mimicked by tiny tools inside the patient’s body.
STAR solved the soft tissue challenge by integrating a few different technologies. Its vision system relied on near infrared fluorescent (NIRF) tags placed in the intestinal tissue; a specialised NIRF camera tracked those markers while a 3D camera recorded images of the entire surgical field. Combining all this data allowed STAR to keep its focus on its target. The robot made its own plan for the suturing job, and it adjusted that plan as tissues moved during the operation.
The researchers trained STAR only on how to perform this particular intestinal suturing procedure. “We programmed the best surgeon’s techniques, based on consensus and physics, into the machine,” Kim said.
An outside expert in the field of surgical robotics called this study a breakthrough, but also said its limitations show that autonomous robots “will not come to the OR soon.” Blake Hannaford, a pioneer of autonomous surgical robotics at the University of Washington, noted that the NIRF tags that the robot relied on were placed by humans.
Hannaford also questioned the clinical significance of the task that STAR performed. “While in a technical sense, semi-autonomous suturing is a ‘grand challenge’ problem of surgical robotics, clinically much suturing and bowel anastomosis is done by staplers which can do the whole thing in seconds,” he wrote in an email. “Clearly the task they chose does not justify the elaborate equipment they used.”
The STAR team said this task was simply intended as proof that autonomous robots could meet the challenge of soft tissue surgery. While the robot may not be ready to take over the OR, Kim said he hopes his technology will be integrated into commercial devices in the next few years. If robotic systems are shown to improve safety and patient outcomes, he said, medicine may go the way of the auto industry.
“Now driverless cars are coming into our lives,” Kim said. “It started with self-parking, then a technology that tells you not to go into the wrong lane. Soon you have a car that can drive by itself.” Similarly, he said, surgical robots could start by giving human surgeons a helping hand. And maybe one day they’ll take over.